Language Barriers in Healthcare: language barriers in healthcare
Discover practical strategies to overcome language barriers in healthcare and improve patient safety, equity, and communication.


When a patient and a doctor can't understand each other, a routine check-up can quickly feel like a high-stakes guessing game. These communication gaps, known as language barriers in healthcare, are far more than a simple inconvenience. They create a breeding ground for misunderstandings, medical errors, and deeply unequal access to care.
For millions of people, this isn't a rare occurrence; it's a constant and dangerous reality.
The Human Cost Of Language Barriers In Healthcare
Imagine the sheer terror of feeling a sharp, unfamiliar pain but having no words to describe it to the one person who can help. That was the reality for Elena, a recent immigrant, when she rushed her young son to the emergency room. He was struggling to breathe, but Elena only spoke Spanish.
Her frantic attempts to explain his history of severe asthma attacks were completely lost on the busy ER staff. Instead of getting the immediate, targeted care he needed, her son's condition was initially misinterpreted. This isn't just a story; it's a daily struggle for a huge portion of the population.
In the United States alone, an estimated 26 million people have limited English proficiency (LEP). A recent KFF survey on racism and health revealed that nearly half of adults with LEP have run into at least one language barrier in a healthcare setting over the past three years.

What These Barriers Truly Mean
The problem runs much deeper than just translating words. Language barriers set off a chain reaction of issues that can compromise every single step of a patient's journey, from booking an appointment to understanding how to take medication after discharge.
The communication breakdown shows up in several critical ways:
- Misunderstood Symptoms: A patient might use a common phrase to describe a symptom that has a very different medical meaning, sending a clinician down the wrong diagnostic path entirely.
- Inaccurate Medical Histories: Without clear communication, how can a patient share vital information about allergies, past surgeries, or family health conditions? They can't.
- Lack of Informed Consent: A patient could end up agreeing to a major procedure without ever truly grasping the risks, benefits, or other options. This fundamentally undermines their autonomy.
- Medication Errors: Confusion over dosage instructions, frequency, or potential side effects can lead to patients taking their medication incorrectly, with potentially devastating consequences.
A language barrier is not just an obstacle in conversation; it's a fundamental flaw in the delivery of care. It transforms the healthcare system from a place of healing into a source of fear, frustration, and inequity for those who cannot make their voices heard.
The Widespread Nature of the Problem
The scale of this challenge is massive. When communication fails, it's not just the patient who suffers—the entire healthcare system feels the impact.
The table below breaks down some of the most common issues LEP patients face, based on data from recent studies. It highlights just how often these critical communication failures occur.
Common Communication Hurdles Faced By LEP Patients
| Challenge Area | Percentage of LEP Patients Affected | Example Scenario |
|---|---|---|
| Communicating with Staff | 33% | A patient cannot schedule a follow-up appointment or ask about a bill because the front desk staff only speaks English. |
| Understanding Provider Instructions | 30% | A doctor explains a complex treatment plan, but the patient only nods along, not wanting to admit they don't understand. |
| Reading Prescription Labels | 25% | An elderly patient takes double the required dose of their blood pressure medication because the instructions were unclear. |
| Filling Out Forms | 22% | A patient leaves critical sections of their intake form blank, omitting key details about their medical history. |
This data shows that these aren't isolated incidents. These barriers are a daily reality in local clinics, pharmacies, and major hospitals across the country. Tackling these language barriers head-on is the first and most critical step toward building a healthcare system that is truly just and effective for everyone.
How Miscommunication Puts Patients at Risk and Deepens Inequity
When a patient and their doctor can't understand each other, the room for error grows with every lost or misunderstood word. These language barriers aren't just minor inconveniences; they are genuine threats to patient safety, turning a routine check-up into a high-stakes gamble. A simple miscommunication can spiral into a serious medical event.
Imagine trying to defuse a bomb with an instruction manual written in a language you don't speak. The pressure is immense, and a single wrong guess could be catastrophic. This is the daily reality for millions of patients with limited English proficiency.
The Direct Link Between Language Gaps and Patient Harm
Breakdowns in communication have a direct, measurable impact on clinical outcomes. When a patient can’t accurately describe their symptoms or a clinician can't clearly explain a diagnosis, the very foundation of effective medicine begins to crumble.
This puts patients in immediate danger in several critical ways:
- Misdiagnosis: If a patient's description of their pain is lost in translation, a doctor might miss the real issue, delaying vital treatment while chasing the wrong problem.
- Medication Errors: A patient could easily misunderstand dosage instructions—like taking a pill twice a day instead of twice a week—leading to an accidental overdose or life-threatening side effects.
- Procedural Complications: True informed consent is impossible without understanding. Patients might agree to a major surgery without grasping the risks, benefits, or other available options.
- Poor Chronic Disease Management: Conditions like diabetes or heart disease demand constant, clear communication about diet, medication, and lifestyle. Language barriers make this ongoing conversation nearly impossible to sustain.
These aren't just hypotheticals. A report from Washington state found that Amharic-speaking patients had a 10% higher mortality rate from sepsis than English-speaking patients. This isn't a statistic; it's a stark reminder that language access is a matter of life and death. Study after study confirms that these communication gaps lead to more serious medical events and longer, costlier hospital stays. You can read more about how breaking language barriers saves lives.
Widening the Chasm in Health Equity
Beyond the immediate danger to individuals, language barriers create a systemic problem that makes existing health inequities even worse. They essentially create a two-tiered system of care: one for English speakers and a lesser one for everyone else.
This unequal playing field hits immigrant and minority communities the hardest, as they often face other significant hurdles in getting good care. When you can't communicate with your doctor, trust erodes, and patients become less likely to seek help or follow through with a treatment plan.
A healthcare system that cannot communicate with all its patients is, by definition, an inequitable one. Language access isn't a "nice-to-have" feature; it's a core component of justice in medicine.
This communication divide leaves entire communities behind, stuck with substandard care that leads to poorer long-term health. The constant stress and frustration of navigating a system that doesn’t speak their language can cause patients to give up, worsening their conditions and straining our healthcare resources even further.
Tackling these language barriers in healthcare isn't just about logistics—it’s a moral imperative. It’s about tearing down a system that privileges one language and ensuring every single patient has the right to be heard, understood, and treated safely.
Meeting Your Legal And Ethical Obligations For Language Access
When a patient with limited English proficiency walks into a clinic, offering them language support isn't just a nice thing to do—it's a fundamental requirement. Failing to provide clear communication isn't just a lapse in care; it's a direct violation of federal law and our core professional duties. This is about much more than checking a compliance box; it's about upholding the very integrity of the care we provide.
The legal bedrock for this is Title VI of the Civil Rights Act of 1964. This is a landmark piece of legislation that forbids discrimination based on race, color, or national origin in any program that gets federal funding. Since most healthcare systems accept Medicare or Medicaid, they are bound by law to give every patient meaningful language access, completely free of charge.
Understanding The Core Mandates
Think of these legal requirements not as a punishment, but as a structural safeguard for quality care. A hospital needs wheelchair ramps for physical access, right? In the same way, it needs language services to ensure everyone has informational access.
The rules are straightforward and non-negotiable:
- Provide Qualified Interpreters: You must offer access to trained, professional medical interpreters. Leaning on a patient's family member or a bilingual staff member from another department is a huge risk—they simply don't have the specialized vocabulary or ethical training needed for complex clinical conversations.
- Translate Vital Documents: Key paperwork, like consent forms, discharge instructions, and information about patient rights, has to be translated into the common languages spoken in your community.
- Inform Patients of Their Rights: You have an obligation to tell patients that language assistance is available to them at no cost, and you have to do it in a language they understand.
These mandates are echoed and reinforced by accrediting bodies like The Joint Commission, which has its own standards for patient-centered communication. Ignoring these responsibilities can lead to devastating consequences, from losing federal funding and facing lawsuits to wrecking your organization's reputation.
The Ethical Imperative Behind The Law
Legal statutes aside, there's a much deeper ethical responsibility at play here. The entire foundation of modern medicine rests on the principles of patient autonomy and informed consent. But for those concepts to mean anything, a patient has to genuinely understand their diagnosis, their treatment options, and the risks they're facing.
Without clear communication, informed consent is impossible. A signature on a form means nothing if the patient behind it never truly understood what they were agreeing to. It transforms a collaborative medical decision into a one-sided directive.
This is where the law and our professional ethics become one and the same. Tackling language barriers in healthcare is an absolute, non-negotiable duty. It's the only way to build the trust needed for a strong patient-provider relationship and to deliver care that is truly safe, effective, and fair for every single person who walks through your doors.
Actionable Strategies For Bridging The Communication Gap
Knowing the risks of language barriers is the easy part. Actually dismantling them is where the real work begins. Healthcare organizations need a multi-layered game plan—one that blends human expertise, smart technology, and a system-wide dedication to clear communication. The goal is simple: build a safety net so no patient’s voice gets lost in translation.
A truly effective strategy is about more than just finding someone who speaks the right language. It’s about weaving a robust language access program into the very fabric of patient care, from the first hello at the front desk to the final conversation in the operating room.
The Human Element: Professional Interpreters And Trained Staff
The absolute bedrock of any language access plan is the use of qualified medical interpreters. These professionals aren't just bilingual; they're specialists trained in complex medical terminology, ethical codes, and the cultural subtleties that can make or break a conversation. They are a precise channel for information, not a filter.
But relying only on professional interpreters isn't always the full picture. Empowering the bilingual staff already on your team can be a huge asset for filling immediate, low-stakes communication gaps. This isn't a free-for-all, though. It requires a formal qualification process to make sure they have the right medical vocabulary and understand the strict ethics of interpreting. Just pulling any bilingual employee into a critical conversation is a recipe for disaster.
Building these skills requires a deep understanding of effective dialogue. While the context is different, many of the core ideas in our guide on cross-cultural communication in business offer powerful insights into navigating these cultural divides.
A professional medical interpreter ensures that a patient's voice is heard exactly as they intend, without alteration or omission. This is a non-negotiable standard for safe and ethical patient care.
This decision tree gives a clear visual breakdown of the fundamental legal duty to provide language access, which is almost always tied to federal funding.
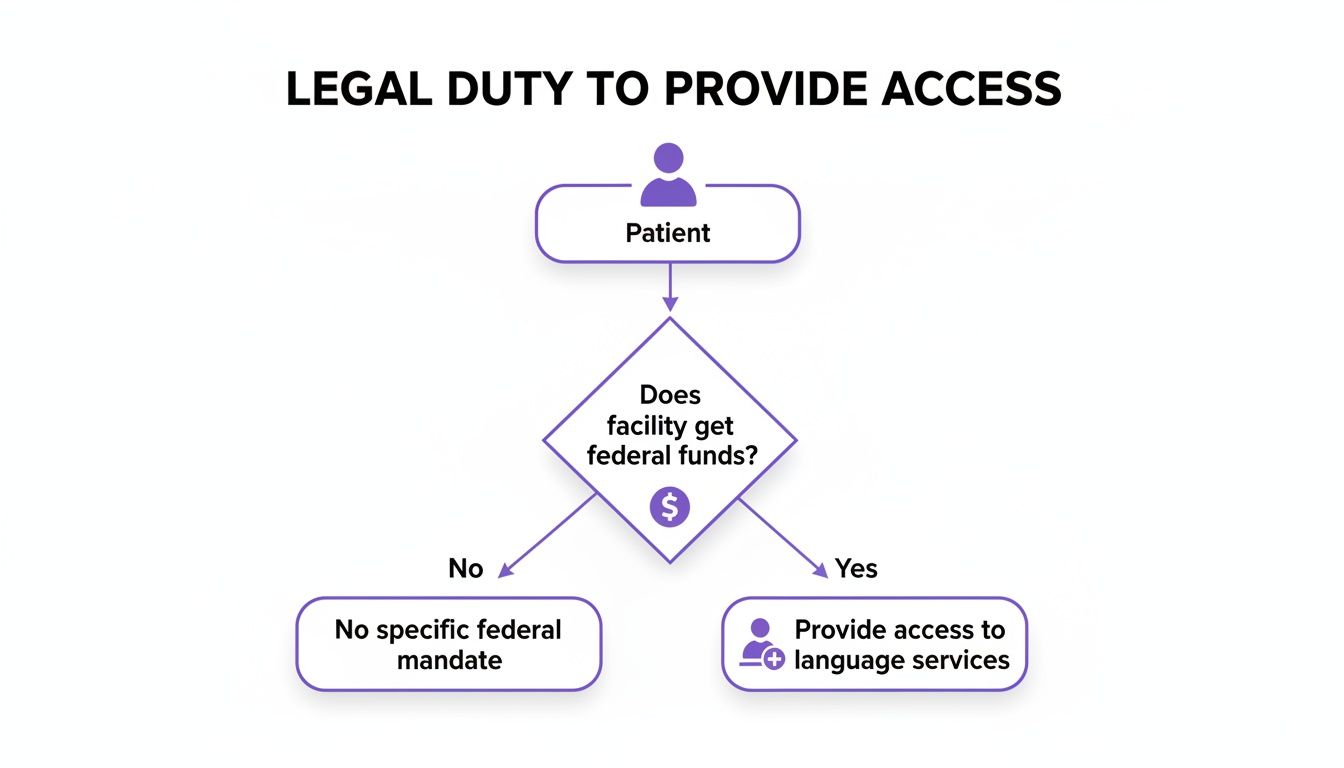
As the flowchart shows, for the vast majority of healthcare facilities, providing language assistance isn't just good practice—it's a legal mandate.
Choosing The Right Interpretation Solution
Not all interpretation methods are created equal. You have to pick the right tool for the job, weighing things like urgency, complexity, and cost. Each approach comes with its own set of pros and cons.
For example, nothing beats an in-person interpreter for a sensitive, end-of-life discussion where you need to read the room and see non-verbal cues. On the other hand, on-demand video remote interpreting (VRI) can be a lifesaver for getting immediate help during a chaotic emergency room visit.
The table below breaks down the most common interpretation services, helping you figure out what makes sense for your facility.
Comparing Language Interpretation Solutions
| Solution | Pros | Cons | Best For |
|---|---|---|---|
| In-Person Interpreters | Highest accuracy; captures non-verbal cues; builds patient trust. | Can be expensive; requires advance scheduling; not always available for rare languages. | Complex diagnoses, surgical consents, mental health, and end-of-life care discussions. |
| Video Remote Interpreting (VRI) | On-demand access; wide language availability; lower cost than in-person. | Requires reliable internet and hardware; may feel impersonal; can be difficult for patients with hearing or vision issues. | Emergency room visits, routine check-ups, and specialty consultations where speed is essential. |
| Over-the-Phone Interpreting (OPI) | Immediate 24/7 access; most cost-effective; largest language selection. | Lacks visual cues, making it harder to build rapport or interpret context. | Scheduling appointments, prescription refills, and simple follow-up questions. |
| Qualified Bilingual Staff | Immediate availability for quick interactions; already familiar with hospital procedures. | May lack formal medical vocabulary; potential for role conflict or emotional bias. | Basic, non-clinical interactions like giving directions or assisting with meal selection. |
Each of these solutions has its place. The key is to have a flexible system that allows clinicians to access the right level of support for any given patient interaction.
The Power Of Plain Language And Cultural Competence
Beyond interpretation services, two other strategies are critical for breaking down language barriers in healthcare.
First, commit to using plain language. Every single patient-facing document—from intake forms to discharge instructions—should be written simply. That means ditching the jargon and overly complex sentences. This helps everyone, not just patients with limited English proficiency.
Second, you have to cultivate cultural competence. This is all about training staff to understand how different cultural backgrounds shape a patient's beliefs about health, their communication style, and their decisions. A culturally aware provider knows how to ask questions with respect and avoid making assumptions, building the trust that’s absolutely essential for effective and equitable care.
Using Technology to Bridge the Communication Gap
Technology is changing the game for how healthcare systems handle language barriers. We now have a powerful set of tools that can connect patients and providers in ways we couldn't before. From instant video calls with interpreters to smart AI platforms, technology is making healthcare more immediate, accessible, and easier to understand.
The goal here isn't just a quick fix. It's about building a system where clear communication is the standard, not a lucky break. When a patient needs help right away, waiting for an in-person interpreter can feel like an eternity. The right tech can collapse that timeline, putting essential resources right at a clinician’s fingertips.
The Rise of Telehealth and Remote Interpreting
The explosion of telehealth has been a massive shift, and many platforms now come with language support built right in. A patient can connect with their doctor from their living room while a professional interpreter joins the video call with a single click. This makes routine check-ups and follow-up appointments so much more accessible for patients who don't speak English fluently.
Beyond telehealth, Video Remote Interpreting (VRI) has become a game-changer inside hospitals and clinics. Picture a nurse in a chaotic emergency room trying to communicate with a distressed patient. Instead of waiting, they can wheel over a cart with a tablet and instantly connect to a live, certified medical interpreter who sees and hears everything. It provides immediate, high-quality communication when every second truly counts.

This setup shows just how seamlessly telehealth can bring everyone into the same conversation, no matter where they are. By putting language support directly into the virtual exam room, these tools break down both geographic and communication hurdles at the same time.
The Promise and Pitfalls of Automated Translation
Let's talk about automated tools. While live interpreters remain the gold standard, apps like Google Translate are often seen as a quick solution in a pinch. But leaning on these generic apps for critical medical conversations is incredibly risky.
They simply lack the deep understanding of medical jargon and cultural nuance that's needed, which can lead to disastrous mistranslations. A machine can't grasp the subtle but critical difference between a "dull ache" and a "sharp pain" the way a trained human can.
However, the world of AI is moving fast. New tools are emerging, and Multilingual AI in Healthcare is starting to make a real difference in patient conversations. These specialized systems are built for clinical settings, offering far better accuracy than any consumer-grade app.
Even with these advances, the digital divide is a major roadblock. Technology is useless if patients can't get to it. It’s shocking, but 29% of hospitals don't offer their patient portals in any language other than English, and a mere 11% provide them in multiple languages. This effectively locks millions of people out of seeing their own test results or scheduling appointments.
Empowering Patients to Become Stronger Self-Advocates
Beyond connecting providers and interpreters, technology can also give patients the tools to take a more active role in their own care. This is where AI-powered learning platforms can make a unique contribution.
Technology shouldn’t just serve providers; it should empower patients. Giving them tools to build their own communication skills fosters independence and helps them navigate the healthcare system with greater confidence.
While professional interpreters are non-negotiable for complex and critical conversations, patients often face smaller, everyday communication hurdles. Think about describing symptoms, scheduling an appointment, or asking a quick question at the pharmacy. Building confidence in these scenarios helps patients become stronger self-advocates and saves professional interpreting resources for the most critical moments.
This proactive approach helps reduce the daily friction caused by language barriers. If you're looking to build these kinds of skills, our guide on the best free language apps can be a great place to start: https://www.talk-easy.com/blog/best-free-language-apps. Empowering patients like this is a key piece of any modern, tech-forward language access strategy.
Building A Successful Language Access Program From The Ground Up
A great language access program doesn’t just appear out of thin air—it’s built with purpose. Getting it right means following a strategic, step-by-step roadmap to design, implement, and measure your efforts. Think of this as a practical guide for creating a sustainable framework that actually moves the needle on health equity.
The first, non-negotiable step is to assess your community’s linguistic needs. Dive into your patient demographic data. What are the primary languages spoken by the people walking through your doors? This information is the bedrock of your entire program, ensuring you put resources exactly where they’re needed most.
Securing Leadership Buy-In and Funding
Once you know what your community looks like, the next hurdle is getting leadership buy-in and a dedicated budget. This is where you have to frame language access as a critical investment, not an expense. It's about patient safety, risk management, and even market growth.
Build a clear business case that shows how breaking down language barriers can decrease adverse events, shorten hospital stays, and boost those all-important patient satisfaction scores.
For organizations looking to fund a new initiative, understanding how to go about securing healthcare grants can be a game-changer. This kind of external support can give your program the strong start it needs.
Implementing and Training Your Team
With leadership on board, you can shift your focus to implementation. And let's be clear: this is about more than just hiring a few interpreters. It requires comprehensive and continuous staff training. Everyone, from the front-desk team to senior surgeons, needs to know how to spot a patient's language need and get them the right help, fast.
Your training should cover the essentials:
- When and how to use professional interpreters in various clinical situations.
- The legal and ethical risks of relying on family members or untrained staff to translate.
- Best practices for clear communication, even when an interpreter is in the room.
Building these skills is an ongoing commitment. Many of the core ideas behind good interpersonal skills are universal, and our article on effective communication skills in the workplace has some great strategies that translate well to clinical settings.
Success isn't just about offering the service; it's about proving its impact. A data-driven approach turns a language access program from a well-intentioned idea into an evidence-based pillar of quality care.
Measuring What Matters Most
Finally, you have to measure your program's performance. Tracking the right key performance indicators (KPIs) is the only way to demonstrate value and find opportunities to improve. You’ll want to focus on metrics that tie language access directly to patient outcomes and operational efficiency.
Here are a few key metrics to keep an eye on:
- Patient satisfaction scores, specifically among LEP populations.
- Rates of medical errors or adverse events, broken down by language.
- Hospital readmission rates for your LEP patients.
- Interpreter utilization rates and how long patients have to wait for one.
By tracking these KPIs, you create a powerful feedback loop. The data not only proves your program’s value but also pinpoints where you can do better. This ensures your system can evolve with your community's needs and truly dismantle language barriers in healthcare for good.
Still Have Questions About Language Access in Healthcare?
When you're trying to navigate healthcare in a language that isn't your own, a lot of questions come up. Let's tackle some of the most common ones that patients, families, and even healthcare providers ask.
Can my family member just interpret for me?
This is a really common question, and it's understandable why people ask. It seems easier and more comfortable to use a family member or friend. However, this is strongly advised against for a few critical reasons, and can even get into hot water with privacy laws like HIPAA.
Think about it: your family members are emotionally invested. They might soften a difficult diagnosis or skip over sensitive questions to protect you, not realizing they're withholding vital information. Plus, medical language is incredibly specific. A professional interpreter knows the precise terminology—a family member, no matter how fluent, usually doesn't.
Professional medical interpreters are trained to be completely accurate, impartial, and confidential. That's the only way to ensure nothing gets lost in translation.
What's the real difference between an interpreter and a translator?
People use these terms interchangeably all the time, but in healthcare, they refer to two very different—and equally important—jobs.
An interpreter works with the spoken word, in real-time. They're the person on the phone, via video, or in the room with you during a doctor's visit, making the conversation flow. A translator, on the other hand, works with the written word. They're the ones who meticulously convert things like consent forms, prescription instructions, or hospital discharge paperwork from one language to another.
In short, interpretation is about a live, spoken conversation, while translation is all about the accuracy of the written word. You need both to truly break down language barriers.
Are hospitals actually required by law to provide interpreters?
Yes, absolutely. In the United States, any hospital or clinic that accepts federal funds—which includes Medicare and Medicaid—is legally required to provide language assistance.
This comes from Title VI of the Civil Rights Act. The law is clear: failing to provide a way for patients with Limited English Proficiency (LEP) to communicate effectively is a form of discrimination. This means offering qualified interpreters and translated documents completely free of charge to the patient.
How does a tool like TalkEasy fit into all this?
While an AI tool can't replace a professional interpreter during a complex medical diagnosis, it can play a powerful role in helping patients feel more prepared and in control.
A tool like TalkEasy helps people practice their conversational English for those everyday healthcare situations. It builds confidence for tasks like calling to schedule an appointment, asking a pharmacist a simple question, or describing symptoms during check-in. This kind of practice empowers patients to become more active, confident partners in their own care.
TalkEasy helps you build the confidence to speak English clearly in any situation. Start practicing today and take control of your conversations with TalkEasy.